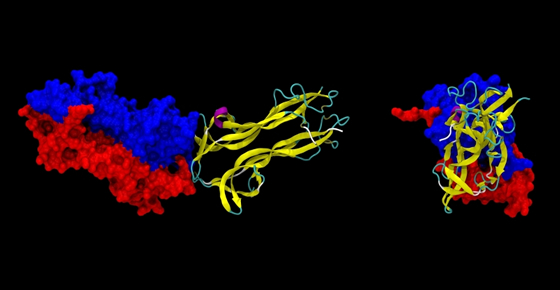
Brain-Derived Neurotrophic Factor
What is BDNF and why is it so important? BDNF stands for brain-derived neurotrophic factor and is a molecule that seems to be responsible for many hea....

Dr. Josuke Tanaka was born and raised in Switzerland. He is a former Swiss national champion in judo and holds a black belt in judo and Brazilian jiu-jitsu.

Dr. Sara Chong has dedicated herself towards building a practice in helping people lead healthier lives by addressing the root causes to their problems.

What is BDNF and why is it so important? BDNF stands for brain-derived neurotrophic factor and is a molecule that seems to be responsible for many hea....

Low level light therapy (LLLT) or photobiomodulation is a therapeutic strategy that has been recently growing in popularity due to the advancement in ....



Stephan ADr. Sara is great! She is knowledgeable, professional, and proved very helpful in dealing with shoulder and ankle injuries I sustained while rock climbing. Her practice is more holistic and wider scope than other chiropractors I know, which allowed me to address diet, sleep, etc as well. A great experience!
Alfred CDr. Tanaka is fantastic!
Dr. Tanaka is very thorough and caring in his treatments. He explains to you about your issues and the progress that is being made.
As a BJJ practitioner I’ve suffered back pains for about 2 years and I went to see two different chiropractors to help solve the issue. However the pain became worse and it went all the way to my hip. After the initial visit with Dr. Tanaka he was able to diagnosis the root cause of the back pain and made me 90% better!
If you are a martial arts practitioner I highly recommend Dr. Tanaka. His martial arts background gives him greater knowledge in understanding and providing a diagnosis and treatment.
Maggie MLong story short… Dr. Tanaka fixed me up in just 2 visits!
A little about my background, I am an athlete and martial artist that trains almost everyday. For the past 2-3 weeks, my left forearm was hurting and numbness shot down from my elbow to my fingers. My necks and shoulders ( upper traps) were also tight and I could not turn my head to the left side . I tried using lacrosse ball, foam roller, stretching, ice, and tiger balm but that only temporary relieved that the pain . Worse of all, it took me away from my training. I was freaking out because I had a Jiu -Jitsu tournament within less than two weeks
Dr. Tanaka got me back to training after my first adjustment. He was very professional, and after some assessments he found the reason behind my weak left arm. It turns out that my back posture was too forward and my muscles were compressing a nerve resulting in numbness, pain, and weakness in my left arm. He adjusted me and prescribed me exercises to fix my posture. After the second visit, my left arm left felt stronger and the pain/numbness was longer there.
If you read his profile, he is also an athlete himself (holds a black belt in Judo and Brazilian Jiu-jitsu) . Some doctors I visited usually advise against training altogether, but Dr. Tanaka understands that athletes need to train and got me back to my normal routine. I cannot thank Dr. Tanaka enough!
C. MI met Josuke at the Guardian gym where he teaches Brazilian jiu jitsu and ginastica natural. First of, he is a great teacher and I encourage you to come train with him at the gym.
During one of the practice classes I popped a rib which took me off the mat for a few weeks.
After just a few sessions with Josuke at the clinic, not only my rib felt way better, but my mobility and strength improved significantly.
I would really recommend Josuke, especially if you practice bjj or any other martial art. As a martial artist himself (he holds black belts in bjj and judo), Josuke like nobody understands the nature of trauma grapplers and fighters get and knows how to treat it.
Also, any other chiropractor or doctor would start telling you that you should give up the sport altogether or just stay away from training as long as possible. Josuke, on the other hand, knows a martial artist’s mentality well and will try to get you in shape as soon as possible, knowing how much being able to train matters to you.Thank you again!